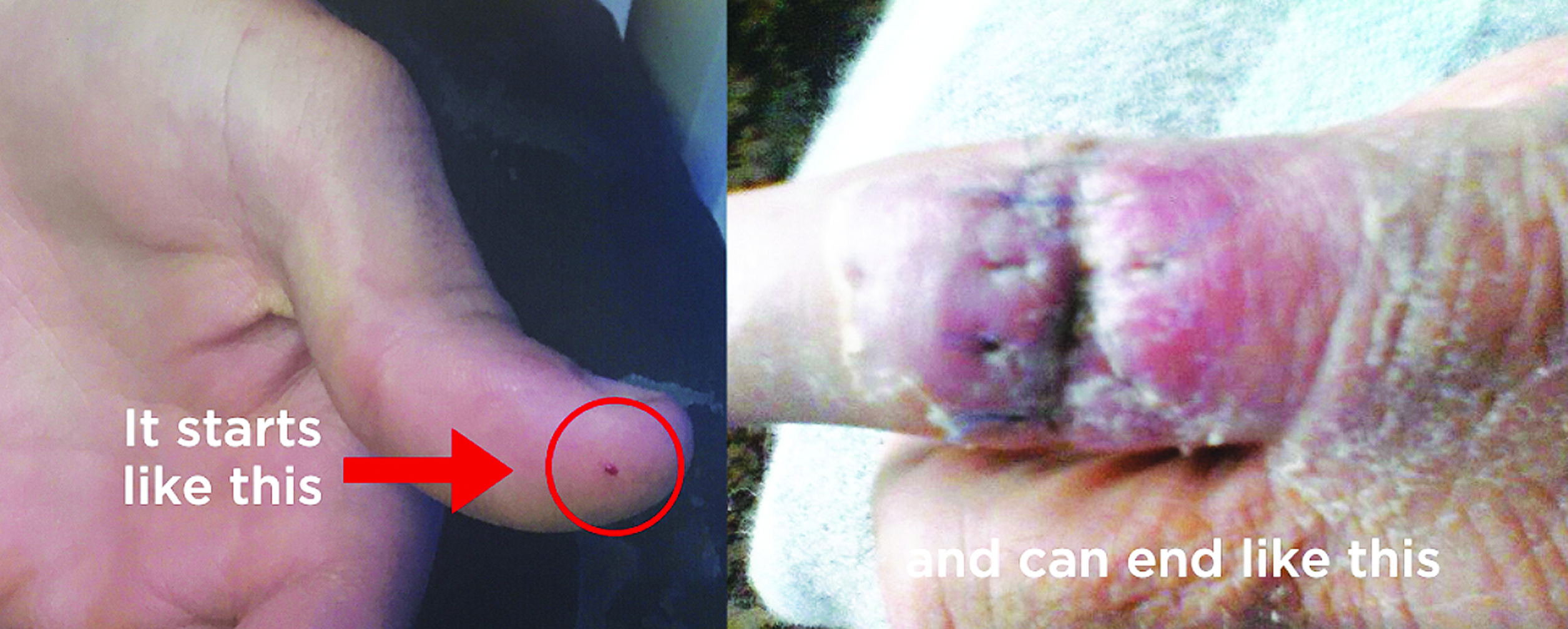
ABOVE: The seriousness of a needlestick injury depends far more on the substance than the needle itself.
NEEDLESTICK injuries are so common in livestock work that they’re often brushed off as part of the job. That’s a mistake. While many are minor, others can lead to serious complications, including permanent tissue damage, systemic poisoning or emergency surgery. For Australian livestock farmers, recognising the difference and responding quickly is what protects you.
Why needlestick injuries matter
Across Australia, the majority of livestock farmers report having experienced a needlestick injury at some point. These incidents typically happen when several risk factors combine – unpredictable animal movement, fatigue, poor restraint, rushed technique or handling high-risk products such as oil-based vaccines. A key problem is delay, both in recognising the seriousness of the injury and in seeking treatment. Many people keep working, assuming it’s nothing. Sometimes it is. Sometimes it isn’t.
First response – stop and assess
If you accidentally inject yourself, don’t push through to finish the job. Stop immediately. Wash the wound thoroughly with soap and water, then take a moment to assess what happened. The level of risk depends on details – what product was involved, how much entered your body and where the injection occurred. A shallow prick is very different from a deep injection into a finger. Before seeking care, gather critical information:
- The product name and label
- The amount injected
- The time of exposure
- Take the container or label with you to the doctor.
Most medical professionals are unfamiliar with livestock pharmaceuticals and treatment decisions rely heavily on knowing exactly what substance is involved. You can also:
- Call the Poisons Information Centre on 13 11 26 for immediate advice
- Contact the product manufacturer using the number on the label
- Access the Safety Data Sheet from the manufacturer’s website.
When to seek urgent medical care
Some exposures should always be treated as urgent. These include:
- Oil-based (oil-adjuvanted) vaccines
- Sedatives such as xylazine
- Hormonal products, for example prostaglandins
- Any injection into a finger, hand or joint
- Increasing pain, swelling, numbness or colour change.
Do not adopt a ‘wait and see’ approach in these cases.

The flyer from the National Centre of Farmer Health contains all the relevant information required for a needlestick injury.
Why some injections are more dangerous
The seriousness of a needlestick injury depends far more on the substance than the needle itself. Oil-based vaccines are among the highest risk. They can trigger severe inflammation and rapidly increase pressure in confined areas such as fingers. This may lead to compartment syndrome, tissue death and surgery if not treated quickly. Sedatives can be dangerous even in tiny amounts. Accidental exposure may cause dizziness, slowed breathing, low blood pressure or collapse. Hormonal products, particularly prostaglandins, can have strong effects on the human body and are especially hazardous for pregnant women. Modified-live vaccines may pose infection risks depending on the organism involved. Antibiotics and long-acting formulations can cause allergic reactions or prolonged inflammation, especially depot (slow-release) products that remain in tissue. The takeaway is simple – never assume an injection is harmless until you’ve identified the product.
Challenges in getting the right treatment
One of the biggest issues in Australia, and globally, is that doctors and emergency departments may not recognise livestock medications or understand their risks. Without clear product information, treatment becomes guesswork. That’s why bringing the label or SDS is so important. It allows healthcare providers to assess toxicity, formulation (such as oil-based versus water-based) and likely complications. Ensuring this information is easy to access – whether in the ute, shed or digitally – is a practical safety step.
Prevention – reducing the risk on farm
While needlestick injuries are common, many are preventable with consistent habits and safer systems. High-risk moments include:
- End of long processing days (fatigue)
- Poorly restrained animals
- Rushed injections or recapping needles.
- Practical ways to reduce risk:
- Avoid recapping needles whenever possible
- Use proper animal restraint every time
- Keep your free hand away from the injection site
- Use the correct needle size for the job
- Dispose of sharps immediately in proper containers
- Consider two-person handling for high-risk products
- Maintain good lighting and safe facilities.
Simple technique changes, such as one-handed vaccination and not ‘tenting’ the skin, can also make a significant difference.
Reporting and follow-up
If a serious exposure occurs, report it. In Australia, incidents involving animal health products can be reported to the Australian Pesticides and Veterinary Medicines Authority. This helps improve safety data and guidance. Health professionals are also encouraged to report adverse outcomes, though they can only do so if they’re aware of the exposure – another reason to clearly communicate what happened.
The bottom line
Needlestick injuries are a predictable part of livestock work, but serious outcomes don’t have to be. The priority is straightforward:
- Stop immediately
- Identify the product
- Seek medical care
- Build safer habits to reduce the risk.
Treat every injection seriously until proven otherwise.